Delivering high-quality care requires more than clinical expertise. It depends on accountability, consistency, and a willingness to look closely at what's actually happening in your records, workflows, and conversations with patients.
Healthcare audits provide a structured way to do that.
They help you identify risks, measure practice against agreed standards, and turn what you find into improvement. Whether the focus is clinical, operational, or patient-facing, audits give clinics a way to spot gaps before they become incidents or complaints.
This guide walks through what healthcare audits are, shows real-world examples, and answers the most common questions.
What is an audit in healthcare?
A healthcare audit is a structured review of clinical practice, operational processes, or organisational systems, measured against an agreed set of standards. The goal is to identify where current practice falls short, understand why, and put changes in place that close the gap.
In practice, healthcare audits serve several purposes at once:
- Improving clinical outcomes by surfacing variation in how care is delivered.
- Ensuring compliance with regulatory, professional, and internal standards.
- Identifying quality gaps in documentation, communication, or workflow.
- Improving efficiency by exposing duplicated effort and bottlenecks.
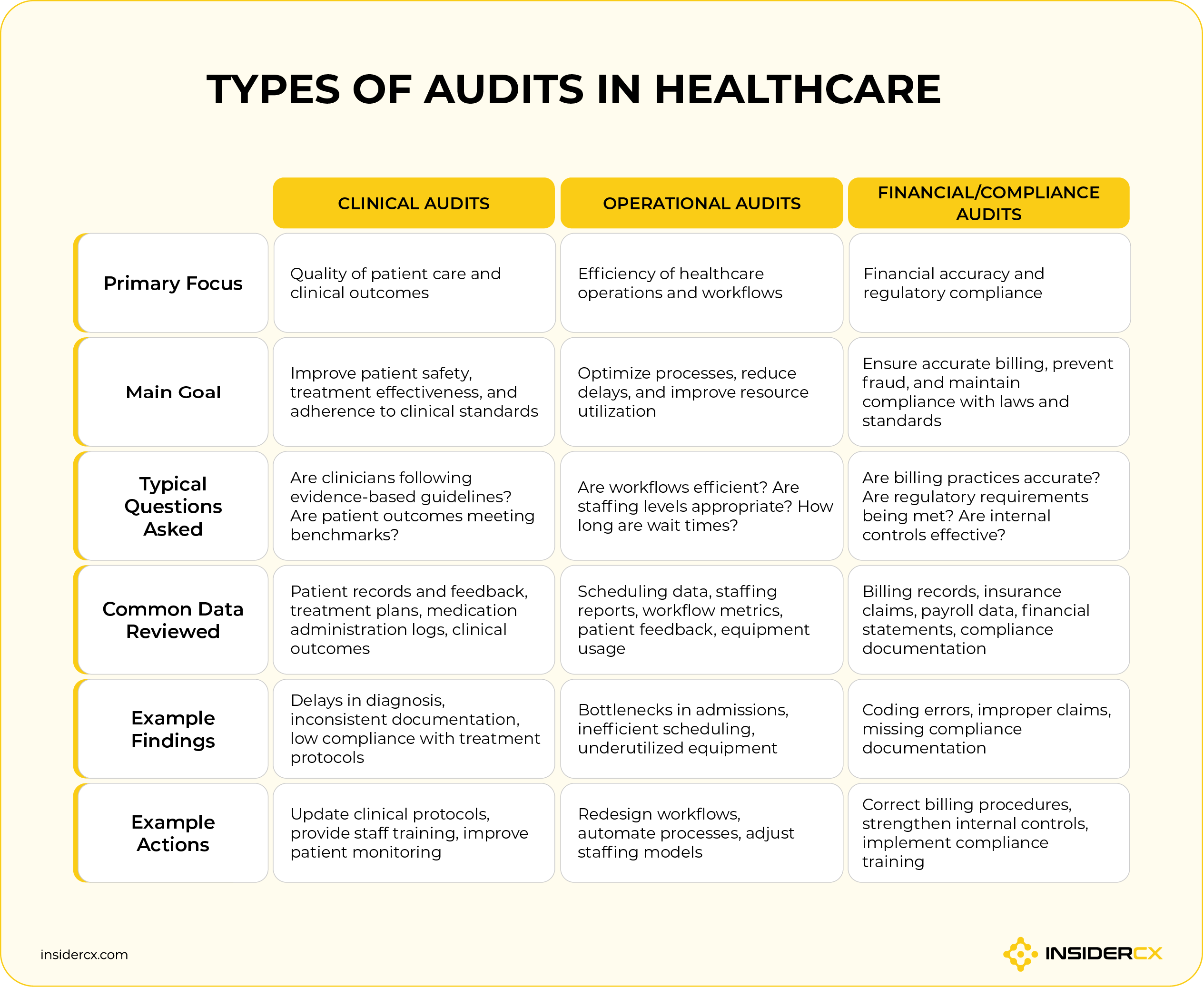
Different audits look at different parts of an organisation. It's helpful to distinguish between three main types of audits performed by clinics and hospitals: clinical audit, operational audit, and financial/compliance audit.
Audits are sometimes confused with inspections, but they're distinct. An inspection is typically external and pass-or-fail — a regulator or insurer checks whether you meet a minimum standard.
An audit, by contrast, is internal, iterative, and specific to your organisation: it measures what you do against what you've agreed you should be doing, and feeds directly into local improvement.
Examples of audits in healthcare
Looking at how audits play out on the ground floor is the fastest way to understand what they actually involve.
The two examples below come from very different settings — one a specialist clinical audit in a histopathology service, the other a non-clinical service-quality audit of the kind a private clinic might run.
Together, they show the breadth of what an audit can cover.
Example #1: An audit to assess the completeness of cervical loop excision histopathology reports
This clinical audit, published by the Royal College of Pathologists, examined how thoroughly cervical loop excision specimens were being reported across UK histopathology services. The published dataset standard for this procedure specifies several core items — including excision type, lesion grade, margin status, and dimensions — that should appear in every report. The audit set out to measure how consistently those items were being recorded and to identify where reporting practice fell short of the agreed standard.
Methods were straightforward but rigorous: participating laboratories submitted anonymised data on consecutive cervical loop excision cases against a structured proforma drawn from the published dataset. That data was then analysed centrally, with each laboratory's results compared against the standards and benchmarked against the wider sample. Both individual and aggregated feedback were returned to participants.
Findings showed broad compliance for some core items but meaningful variation for others, particularly around the recording of margin status and dimensions. Recommendations focused on tightening local reporting templates, raising awareness of the dataset's minimum requirements, and re-auditing after a defined interval to confirm that the changes had taken hold.
Example #2: A patient experience and efficiency audit in a private dental clinic
The clinic's leadership team had noticed a slow drift in returning-patient rates and a rise in negative comments about waiting times in online reviews. They commissioned an internal audit to assess the patient experience end-to-end — from the first enquiry through to post-treatment follow-up — and to identify the operational drivers behind the trend.
The audit combined several feedback streams:
- Post-visit feedback surveys were sent to every patient within 24 hours of their appointment, with both NPS (Net Promoter Score) and open-text questions.
- A sample of patients was invited to short telephone interviews for richer detail.
- Online reviews from the previous 6 months were coded thematically.
- Operational data was pulled from the practice management system and matched against the feedback dates.
Three patterns emerged:
- The average waiting time on arrival had crept from 7 minutes to 16 minutes over the period, driven largely by over-scheduling on certain clinicians' lists.
- Patients who had a hygienist appointment immediately followed by a clinical consultation reported significantly lower satisfaction, because the handover felt rushed and the second clinician didn't always reference the hygienist's notes.
- Post-treatment follow-up was inconsistent — some patients received a courtesy call the next day, others heard nothing at all.
The clinic adjusted scheduling templates to build in realistic buffer time, introduced a structured handover note between clinicians who saw the same patient on the same day, and standardised a 24-hour follow-up message after any treatment.
The point of this example isn't the specifics, it's the shape. A non-clinical audit can be every bit as rigorous as a clinical one, and in a private healthcare setting, it often has the most direct impact on patient retention and reputation.
The role of patient feedback in healthcare audits
Quantitative data (like the NPS score or the average wait times) tells you what is happening. And patient feedback tells you why.
Audits that rely only on operational metrics or clinical records often miss the texture of the patient experience — the things that drive satisfaction, complaints, and ultimately whether someone comes back or recommends you to a friend.
Feedback used in audits can come from several sources, each with a different strength:
- Satisfaction/feedback surveys: Structured, comparable across patients and time, well-suited to tracking change.
- Online reviews and comments: Unprompted, public, often the first sign of a recurring issue.
- Official complaints: Small in volume but high in signal; each one usually points to a process gap
- Interviews and focus groups: Slow but rich; the best way to understand the "why" behind a trend.
When used alongside clinical and operational data, patient feedback adds dimensions that no internal metric can capture. It:
- Surfaces issues that don't appear in the records — a clinician's tone, the cleanliness of a waiting area, the clarity of pre-procedure instructions.
- Validates or challenges what the numbers suggest — a clinic might hit its appointment-time targets and still hear that visits feel rushed.
- Uncovers patterns across touchpoints — a single complaint about post-treatment communication is anecdote; twenty complaints across three months is a system problem.
- Gives clinicians and managers a shared reference point — concrete patient quotes carry weight in a way that aggregate scores don't.
- Feeds the re-audit cycle — tracking patient sentiment before and after a change is one of the clearest ways to show whether the change actually worked.
The clinics doing this well treat patient feedback as audit evidence on equal footing with the clinical record: captured systematically, analysed alongside other data, and built into every review.
How to conduct an audit in healthcare?
At a high level, a healthcare audit follows a defined cycle. You identify a topic where practice could be improved or where variation is suspected. You agree on the standards you'll measure against, usually drawn from guidelines, regulations, or internal policy. You then collect data on current practice and compare it to those standards.
Where you find gaps, you put an action plan in place. After a defined interval, you re-audit to check whether the change has held.

For a deeper walk-through of each step, including how to scope a topic, set measurable criteria, and design the action plan, see our full guide to running a clinical audit.
How InsiderCX helps clinics and hospitals streamline the audit process
Most clinics don't find value in audits because they lack the will to do them — they seem ineffective because the data is scattered. Patient feedback sits in one system, operational metrics in another, online reviews in a third.
Pulling it all together for an audit means weeks of manual collection, and by the time the picture is assembled, the moment for timely action has passed. Plus, when the changes are implemented, it’s difficult to quantify their effects.
InsiderCX is built to remove those frictions:
- Centralised patient feedback brings surveys, reviews, complaints, and interview notes into a single platform, making them searchable, taggable, and tied to specific touchpoints in the patient journey.
- AI-powered sentiment analysis automatically goes through all open-ended feedback and identifies how patients feel about every major touchpoint in the patient journey.
- Real-time detractor alerts and the ticketing system help systematically catch and resolve emerging issues, rather than waiting for the next audit window.
- Automated reporting turns weeks of manual compilation into a few clicks, with audit-ready summaries broken down by site, clinician, service line, or time period.
When done right, an audit is less a project and more an ongoing rhythm, a continuous loop between what patients tell you, what your data shows, and what you change as a result. That rhythm is what InsiderCX is designed to support.
If you'd like to see how this works on real clinic data, book a product demo. We'll walk through how InsiderCX fits into your current audit cycle and what the setup would look like in your organisation.
FAQs
What is the purpose of an audit in healthcare?
The purpose of a healthcare audit is to measure current practice against agreed standards, identify gaps, and drive improvement. In a well-run clinic, audits are the main mechanism for quality improvement (QI), covering clinical outcomes, compliance, efficiency, and the patient experience.
What is an audit trail in healthcare?
An audit trail represents a chronological record of every action taken on data or within a system — who did what, when, and why. Audit trails are essential for clinical records, prescribing systems, and patient experience platforms, supporting both accountability and GDPR compliance.
What are the differences between internal and external healthcare audits?
Internal audits are run by clinics themselves, focused on local improvement. External audits are run by an outside body — a regulator, insurer, or accreditation organisation — and tend to be formal and compliance-focused. Most healthcare organizations use both.
Who should lead internal audits in clinics and hospitals?
In healthcare groups, a quality manager, clinical governance lead, or audit committee will lead internal audits. In smaller private clinics, it can be done by a senior clinician with operational responsibility or the clinic manager. Whoever does it should have the authority to act on the findings.
How often should I conduct an audit in my private practice?
At least one focused audit per year on a specific topic, with a re-audit 6–12 months after the action plan is in place. Patient experience audits, which rely on continuous feedback, can run on a rolling basis with quarterly reviews.
How long does a healthcare audit take?
Most audits run 4–12 weeks end-to-end. Multi-site audits can take longer, while re-audits are usually faster because the standards and tools are already set. The bulk of the time goes to data collection, which is exactly where a structured platform shortens the timeline.
What is a retrospective audit in healthcare?
The majority of healthcare audits are retrospective audits. They are conducted after patient care, treatment, or billing activities have already occurred. The contrast is a prospective audit, which collects data on cases as they occur. Retrospective audits are faster to run; prospective audits offer cleaner data and a tighter feedback loop.
Who offers the best audit practices for healthcare?
For clinical audit guidance, look to professional bodies and national frameworks: the Royal Colleges in the UK, the Healthcare Quality Improvement Partnership (HQIP), and dedicated sites like the Clinical Audit Support Centre. For the operational and patient-experience side, purpose-built platforms like InsiderCX provide the infrastructure to run audits continuously rather than as one-off projects.