Every clinic collects some form of patient feedback, but only a few do something meaningful with it. Surveys go out, scores come back, and the data sits in a spreadsheet — occasionally referenced, rarely acted on.
Patient feedback analysis is the process of organising, segmenting, and interpreting patient responses to identify patterns, root causes, and opportunities for improvement across your services. When done right, it becomes an integral part of quality management.
This article walks you through a proven framework for analysing patient feedback — from building the right foundation with smart surveys, through the analysis process, to turning insights into measurable improvements.
It all starts with smart patient surveys
Before you can analyse feedback, you need feedback worth analysing. That means collecting it in sufficient volume, with minimal bias, and in a format that lends itself to structured review.
Instead of relying on comment cards or ad hoc questionnaires, think automated, well-designed survey programmes that generate a consistent flow of usable data.
Automating the process — sending surveys via SMS or WhatsApp within 24–48 hours of a visit — removes the burden from staff and dramatically increases response rates. But automation alone isn't enough; the quality of your survey design determines the quality of incoming feedback.
Well-designed, properly worded, and strategically timed surveys make a measurable difference:
- Neutral, unbiased wording prevents skewed responses: Leading questions like "How much did you enjoy your visit?" push patients toward positive answers. Neutral phrasing — "How would you rate your overall experience?" — produces data you can trust.
- A mix of quantitative and qualitative questions gives you both the numbers and the narrative: Closed-ended questions (rating scales, NPS) let you track trends; open-ended follow-ups let patients explain why they gave that score.
- Targeted questions mapped to the patient journey surface specific, actionable insights: Rather than asking broadly about "your experience", asking separately about scheduling, wait times, staff communication, and aftercare helps you find root causes of dissatisfaction.
- Short, focused surveys improve completion rates without sacrificing depth: Surveys that take two to three minutes to complete consistently outperform longer ones — patients are more willing to respond, and the data stays focused.
- Conditional logic keeps surveys relevant to each patient: Branching questions — where follow-ups depend on previous answers — ensure patients only see questions that apply to their experience, reducing friction and improving data quality.
If you're still designing surveys from scratch without expert input, it's worth exploring how a well-designed patient feedback form can improve both response rates and the quality of those responses.
The proven patient feedback analysis framework
With a solid survey programme in place, you will have enough objective feedback for a proper analysis. The six steps below outline how to do it.

Step 1: Consolidate and organize patient feedback data
Before analysis can begin, feedback must be centralised and structured. Patient feedback typically arrives from multiple channels — surveys, online reviews, comment boxes, emails, and call centre transcripts. When this data lives in separate systems, it's nearly impossible to spot patterns or compare across departments.
Key best practices for this stage:
- Consolidate feedback into a single analytics platform or database so nothing falls through the cracks and all data is accessible in one place.
- Standardise data formats to make responses comparable — especially when pulling from different survey tools or collection methods.
- Separate structured data (ratings, scores) from unstructured data (free-text comments) so each type can be analysed with the right approach.
- Tag feedback by department, location, provider, or service line to enable the segmentation that makes analysis actionable.
- Remove duplicate or incomplete responses where necessary to keep your dataset clean.
In practice, most — if not all — of this can be automated by using a patient experience platform like InsiderCX. These platforms can consolidate survey responses, review scores, and complaint records into a single dashboard, automatically categorising incoming feedback so your team can skip the manual data wrangling and move straight to analysis.
Step 2: Segment feedback by patient journey stage
Analysing feedback in aggregate can hide crucial insights. A clinic-wide satisfaction score of 8.2 does not tell you where patients are having good or bad experiences. Segmenting responses by where they occur in the patient journey helps pinpoint exactly which touchpoints are driving satisfaction — or complaints.
Common segmentation categories include:
- Appointment scheduling: Ease of booking, availability of preferred times, confirmation process.
- Waiting room experience: Actual vs. expected wait times, comfort, communication about delays.
- Interaction with medical staff: Bedside manner, clarity of explanations, time spent with the patient.
- Communication and explanations: How well staff conveyed diagnoses, treatment options, and next steps.
- Treatment or procedure experience: Pain management, professionalism, perceived quality of care.
- Billing and administrative processes: Transparency of costs, ease of payment, follow-up invoicing.
- Post-visit follow-up: Aftercare instructions, check-in calls, ease of reaching the clinic with questions.
This step allows healthcare teams to identify which touchpoints drive positive or negative experiences — and focus their improvement efforts accordingly.
Step 3: Quantify patient satisfaction metrics
Structured survey responses make it possible to track measurable indicators of patient experience over time. This is where your quantitative data earns its keep.
Common metrics to analyse include:
- Overall satisfaction score: The broadest measure of how patients perceive their experience.
- Net Promoter Score (NPS): A single-question metric that gauges how likely patients are to recommend your clinic, widely used as a benchmark for patient loyalty.
- Provider communication ratings: How patients evaluate the clarity and empathy of their interactions with clinical staff.
- Wait time satisfaction: One of the most frequently cited sources of patient frustration.
- Staff professionalism ratings: Covering reception, nursing, and administrative teams.
Once you're tracking these metrics consistently, look for:
- Trends over time: Is satisfaction decreasing, improving month over month, or plateauing? A steadily declining NPS, for example, signals a systemic issue that needs attention.
- Differences between departments or providers: Comparing scores across teams can reveal which departments are excelling and which need support. One clinic may find that surgical satisfaction is consistently high while outpatient communication scores lag behind.
- Sudden drops in key metrics: A sharp dip in a specific score often points to a recent operational change, staffing issue, or process failure worth investigating immediately.
- Gaps between locations or services: For multi-site organisations, location-level benchmarking highlights where best practices exist and where they need to be replicated.
Quantitative analysis highlights where performance is improving — and where attention is needed. We already have a resource that is a useful companion to this framework, in case you need guidance on measuring and improving patient satisfaction.
Step 4: Analyze qualitative feedback using themes and sentiment
Open-ended comments often contain the most valuable insights, but they require structured analysis to be useful at scale.
A hundred free-text responses scattered across a spreadsheet won't tell you much. However, the same hundred responses, categorised by theme and sentiment, can reveal exactly what's driving your scores up or down.
Methods for analysing qualitative feedback include:
- Sentiment analysis (positive, neutral, negative): Classifying the emotional tone of each response to quickly gauge overall patient mood and spot problem areas.
- Theme categorisation: Grouping comments by recurring topics such as "wait time", "communication", "billing", or "staff attitude".
- Grouping comments by recurring issues or praise: Identifying the most frequently mentioned positives (to reinforce) and negatives (to address).
- Flagging outlier responses: Individual comments that describe particularly poor or particularly outstanding experiences, which can point to staff training opportunities or best-practice examples.
Common patient feedback themes include long waiting times, poor communication or unclear explanations, staff friendliness and empathy, facility cleanliness, and administrative complexity.
Again, you will need a patient experience survey software like InsiderCX to do this at scale. Here’s a quick example of how the algorithms sort and categorise feedback in the background:
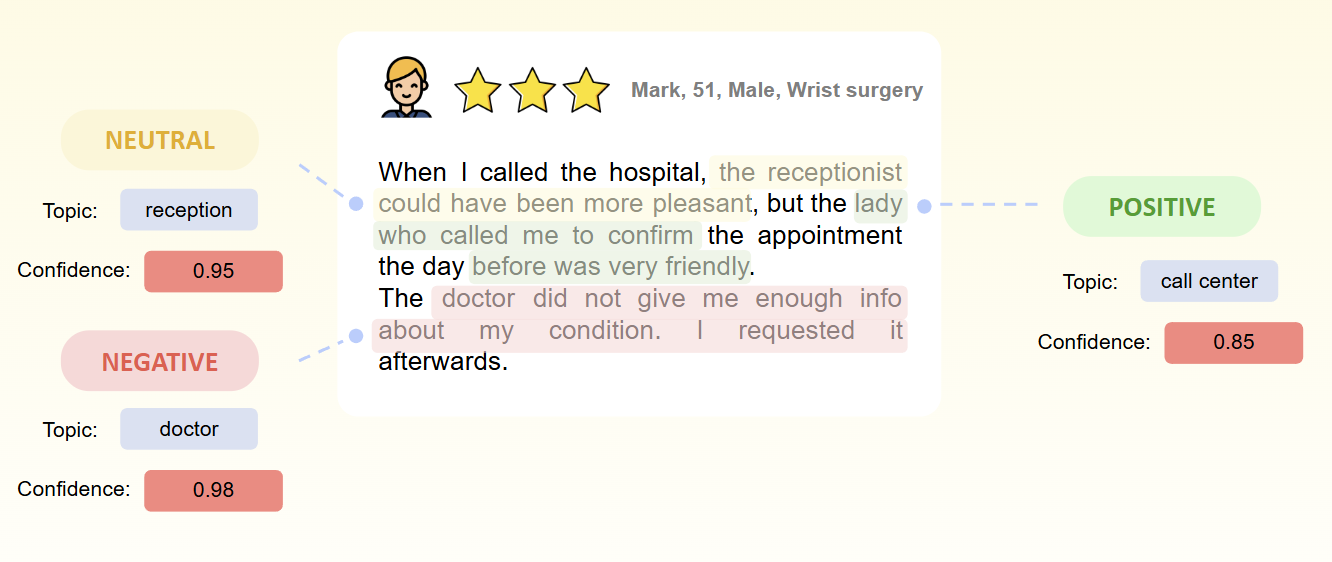
And here is a screenshot of a dashboard in InsiderCX, where healthcare organizations can see all (green), neutral (orange), and negative (red) sentiment tied to different aspects of their patient journey. This saves clinics hundreds of hours they would otherwise have to spend reading and categorising feedback.
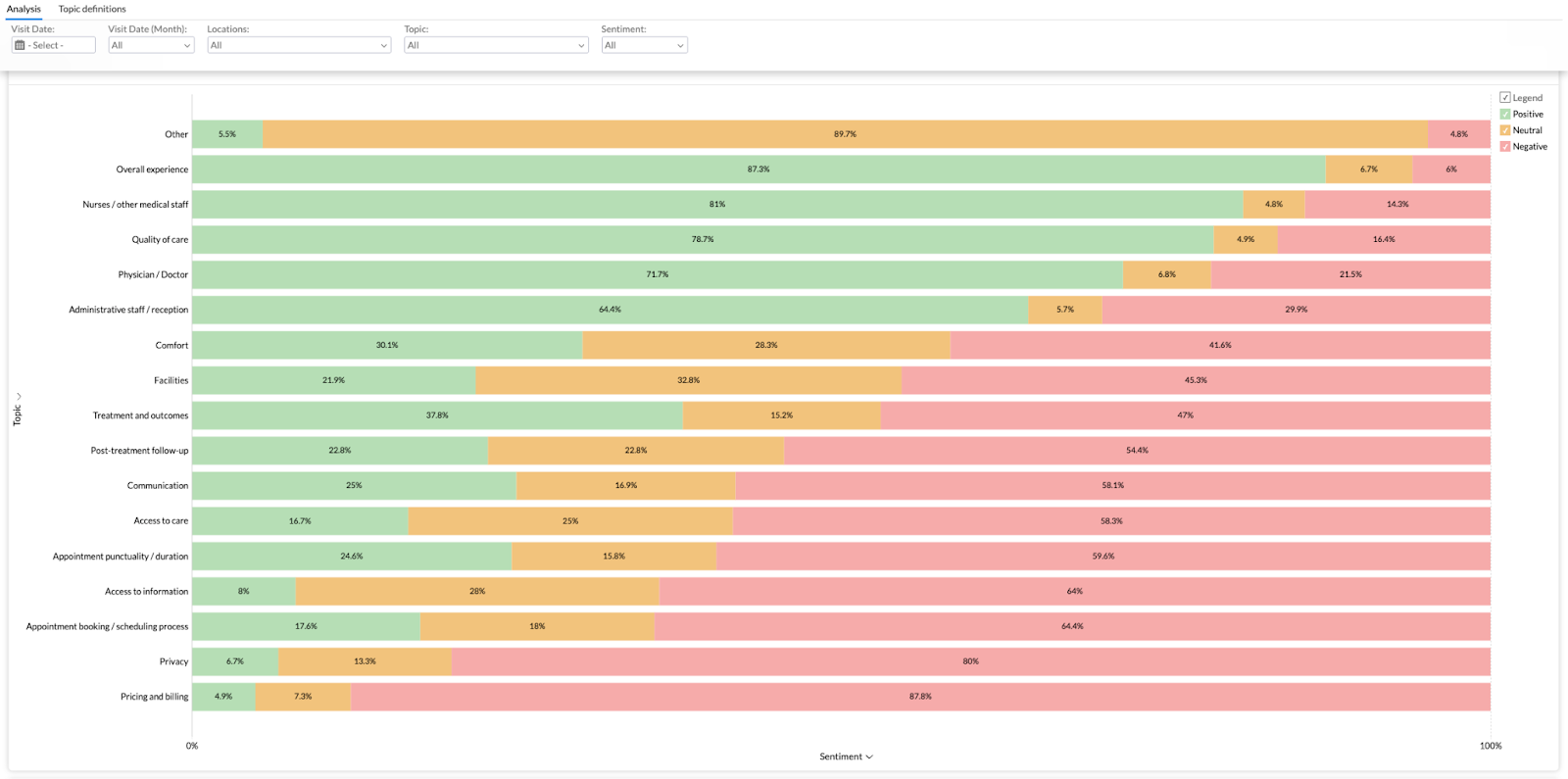
TL;DR: Qualitative analysis helps explain why certain satisfaction scores are high or low, which is something the numbers alone can't do.
Step 5: Identify root causes behind recurring issues
At this stage, the goal is to move from symptoms to causes. Surface-level complaints often point to deeper operational problems, and fixing the symptom without addressing the root cause means the same issue will keep reappearing in next month's feedback.
For example:
- Complaints about wait times may indicate scheduling inefficiencies — not simply a need for faster service, but perhaps an overbooking pattern or a bottleneck at a specific stage of the visit.
- Negative communication feedback may point to training gaps — or it may reveal that doctors are under time pressure and cutting consultations short.
- Billing complaints may reveal confusing administrative processes — unclear pricing, unexpected charges, or invoices that don't match what was discussed during the visit.
Helpful techniques for getting to the root cause:
- Root cause analysis (5 Whys): Ask "why" five times in succession to peel back the layers. Why are patients complaining about wait times? Because appointments are running behind. Why? Because the intake process takes too long. Why? Because forms are filled out on paper at the reception. And so on.
- Cross-referencing feedback with operational data: Compare patient complaints about delays with actual scheduling data to determine whether the problem is capacity, staffing, or process-related.
- Comparing results across departments or time periods: If one department consistently outperforms another on the same metric, the difference likely points to a process or leadership factor. Investigate it.
- Reviewing outlier responses in detail: Extreme negative or positive responses often contain the most specific, actionable information about what's going right or wrong.
This step ensures healthcare organisations focus on the underlying operational issues rather than off-the-cuff complaints.
Step 6: Prioritize improvement opportunities
You can’t address all issues at once. Resources are finite, and trying to fix everything simultaneously usually means nothing gets fixed well. Healthcare organisations should prioritise improvements based on impact and feasibility.
Consider the following:
- Frequency of the issue: How often does it appear in feedback? A problem mentioned by 40% of respondents demands more urgency than one mentioned by 3%.
- Severity of patient dissatisfaction: Some issues generate mild annoyance; others cause patients to leave and never return. Weight accordingly.
- Impact on patient safety, care quality, or compliance: Anything that affects clinical outcomes, safety, or compliance takes precedence, regardless of frequency.
- Operational complexity and financial cost of solving the issue: Some high-impact improvements are surprisingly low-cost (updating a communication template, for instance), while others require significant investment.
- Alignment with organisational goals: Improvements that support broader strategic priorities, such as patient retention, reputation management, and accreditation, should be prioritised over isolated fixes.
Some clinics use a simple impact vs. effort matrix to determine which improvements should be tackled first.

Plot each issue on two axes — patient impact (high to low) and implementation effort (easy to hard) — and start with the high-impact, low-effort quadrant. Just be careful, organizations tend to underestimate effort and overestimate impact.
Acting on the results of patient feedback analysis
The purpose of patient feedback analysis is to spot problems and areas for improvement. Analysis without action is a wasted investment. The real value comes from closing the loop: turning insights into changes, communicating those changes to staff, and monitoring whether the improvements stick.
A closed-loop feedback process means that every piece of actionable feedback triggers a defined response, whether that's resolving an individual patient's concern, updating a process, or escalating an issue to leadership. When patients see that their feedback leads to visible change, they're more likely to provide it again — and more likely to stay loyal.
Here's a practical framework for continuously translating patient insights into quality improvements:
- Assign ownership for every category of feedback: Complaints about billing go to the admin lead, clinical feedback goes to the medical director, and so on.
- Set up real-time alerts for critical feedback: Don't wait for the monthly report to learn about a seriously dissatisfied patient. Set up instant detractor alerts so teams can intervene before the patient is lost.
- Hold regular review sessions: Weekly huddles keep staff aligned on emerging patterns; monthly reviews give leadership the data they need to make resource decisions. Structured feedback reports make these sessions more productive and less anecdotal.
- Track the impact of every change you make: If you adjust your scheduling process based on wait-time complaints, monitor the relevant scores for the next 8–12 weeks to determine whether the change had the desired effect.
- Communicate improvements back to patients and staff: Let patients know their feedback mattered through signage, email updates, or a brief note in the next survey. Internally, celebrate the wins so staff see feedback as a constructive tool, not a punitive one.
- Repeat the cycle continuously: Patient feedback analysis isn't a quarterly project — it's an ongoing operational discipline. The clinics that improve fastest are the ones that treat this as a regular rhythm, not an occasional exercise.
InsiderCX — the top patient feedback analysis platform for private healthcare
InsiderCX is a patient experience platform designed specifically for private clinics and hospital groups. It handles the entire feedback lifecycle, from survey design and automated collection through to analysis, reporting, and closed-loop follow-up. Healthcare teams can focus on acting on insights rather than gathering them.
Key InsiderCX features that streamline patient feedback analysis:
- Expert survey design by domain specialists: Our team helps clinics develop questionnaires grounded in healthcare best practices, ensuring better-quality data and higher response rates.
- Automated, multi-channel feedback collection: Surveys are sent automatically via SMS or WhatsApp within 24–48 hours of a patient visit, consistently generating the volume of feedback needed for reliable analysis.
- Built-in sentiment analysis: Open-ended patient responses are automatically classified by sentiment and theme, surfacing recurring issues without manual review.
- Comprehensive feedback analytics dashboard: All quantitative and qualitative data is accessible in one place, segmented by department, provider, location, service, or time period.
- Weekly and monthly progress reports: Dedicated account managers deliver structured reports that track key metrics, highlight emerging trends, and recommend specific actions for improvement.
- Real-time detractor alerts and ticketing: Negative feedback triggers immediate notifications so teams can respond quickly. There is also a built-in ticketing module with custom SLAs to track and speed up resolution.
- Online reputation management: Satisfied patients are automatically prompted to leave reviews on Google or Trustpilot, helping you improve your review scores along the way.
Schedule a demo to learn more about the InsiderCX platform and our completely free pilot project.
Frequently asked questions
What are the best tools for analysing patient feedback?
The best patient feedback analysis tools combine automated feedback collection with built-in analytics, including sentiment analysis, trend tracking, and segmentation by department or provider. Dedicated patient experience platforms like InsiderCX are purpose-built for healthcare and offer end-to-end capabilities. General-purpose survey tools can work for smaller operations, but they typically require more manual effort to organise and interpret the data.
How often should patient feedback analysis be performed?
Continuously, with structured reviews at regular intervals. In practice, this means monitoring incoming feedback in real time (especially detractor alerts), conducting weekly reviews with frontline teams, and running deeper monthly or quarterly analyses for leadership. The cadence depends on your patient volume — high-volume clinics benefit from more frequent review cycles.
Who should conduct patient feedback analysis?
Quality managers or patient experience leads are typically responsible for the analysis itself, but the results should be shared across the organisation. Clinical feedback should reach medical directors and department heads; operational feedback should involve admin and scheduling teams. The most effective clinics build a culture where feedback review is a shared responsibility, not a siloed function.
How does patient feedback collection and analysis help with compliance?
Systematic feedback collection and analysis create a documented record of patient concerns and the actions taken to address them. This is increasingly relevant for accreditation bodies and regulatory frameworks that require evidence of continuous quality improvement. A structured feedback programme demonstrates that your organisation listens to patients, tracks outcomes, and makes measurable changes — all of which support compliance with standards like CQC, JCI, or ISO 9001.




